- Suggests how to improve treatment outcomes
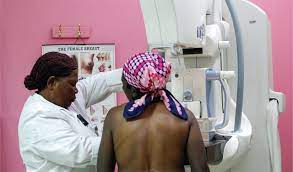
Genetic variants, CYP2D6*17 and CYP2D6*29, found in black patients with breast cancer are associated with a significant reduction in the effectiveness of a breast cancer drug. Dose escalation in the patients could result in an improved treatment outcome, two new studies have shown.
Collen Masimirembwa, the chief scientific officer of the African Institute of Biomedical Science and Technology (AiBST), Zimbabwe, and colleagues, in two studies on Zimbabwean and South African populations, have shown that as many as 48% of African breast cancer patients did not retain therapeutically effective levels of endoxifen, the active component of the drug tamoxifen, and that these women carried African-specific genetic variants which made them an intermediate metaboliser (IM).
Black African women with breast cancer have a low survival rate because the treatment they receive is not formulated to take into account their genetic composition and variability. Pharmacogenetics evaluates the impact of genetic variation on patient response to treatment. Researchers are beginning to understand how African genetic variation affects the metabolism and treatment outcomes of tamoxifen, an affordable and widely used hormone therapy for women with oestrogen receptor-positive breast cancer.
Despite its proven clinical effectiveness, research in European and Asian populations has shown that tamoxifen treatment efficacy can be influenced by age, drug-drug interaction, drug resistance and genetic polymorphisms of enzymes involved in the metabolic pathway of the drug.
Masimirembwa has been studying genetic variation in CYP2D6 – an enzyme expressed in the liver, which catalyses reactions involved in drug metabolism and synthesis. He discovered an African specific variant called CYP2D6*17 that occurs in more than 30% of African populations and is practically absent in other world populations. Researchers are still unravelling the impact of genetic polymorphism in CYP2D6 enzyme activity and how co-medications for other chronic conditions affect patients of African descent with breast cancer.
“We found that doubling the dose of tamoxifen (from the standard dose of 20 mg/day to 40 mg/day) would result in these individuals having effective concentrations of the active compound,” says Comfort Kanji, of the African Institute of Biomedical Science and Technology (AIBST), Zimbabwe, who co-lead one of the studies.
The authors suggest that more studies need to be done to reach a consensus on how best to use CYP2D6 genotypes as predictors for patients who can benefit from dose adjustment. In the South African study the researchers investigated the effect of co-medication in a cohort of 229 Black South African female patients with hormone-receptor positive breast cancer who had been concurrently on antiretroviral therapy (ART) for HIV for at least three months.
The findings showed no clinically significant risk of drug-drug interactions in these patients taking tamoxifen and efavirenz-based antiretroviral therapy.